Mixed-effects multivariate regression models were used to analyse longitudinal data. Independent variables ( Table 1) were obtained from a thorough medical history and medical records, and included demographic information, comorbidities featuring as active diagnoses in the patients’ electronic medical records and coded using the ICD-10, medication used to treat vertigo, and other medication of interest.ĭata were analysed in accordance with the Consolidated Standards of Reporting Trials (CONSORT) guidelines, 20 and comparisons between groups were based on the intention-to-treat principle.ĭescriptive statistics were used for all of the study variables, and cross-sectional differences were analysed between the intervention and sham groups using the Wilcoxon test for continuous variables and Fisher’s exact test for categorical variables. Self-reported vertigo severity assessed on a 10-point Likert-type scale ranging from 0 (no dizziness) to 10 (worst imaginable dizziness).Īll the outcome variables were assessed at 1-week, 1-month, and 1-year follow-up visits. Self-reported resolution of vertigo assessed by a ‘yes/no’ answer to the question: ‘Have you experienced vertigo this week?’ Positive results were further divided into a positive result for both vertigo and nystagmus (positive DHT with nystagmus), and a positive result for vertigo only (positive DHT without nystagmus). Responses were classified as negative (neither vertigo nor nystagmus) or positive.
#Vertigo maneuver plus
The authors therefore removed patients who met criteria a plus b or c. The diagnosis is considered probable when either criteria b or c is fulfilled. Not better accounted for by another vestibular or ICHD diagnosis. Headache with at least two of the following characteristics: one-sided location, pulsating quality, moderate or severe pain intensity, or aggravation by routine physical activity
One or more migraine features, with at least 50% of the vestibular episodes: 18 These are:Īt least five episodes with vestibular symptoms of moderate or severe intensity, each lasting 5 minutes to 72 hours.Ĭurrent or previous history of migraine, with or without aura, according to the International Classification of Headache Disorders (ICHD). Thus, on completion of the recruitment and follow-up phases, the authors reassessed all patients and removed those who met the newly defined criteria established for probable vestibular migraine in 2013.
#Vertigo maneuver trial
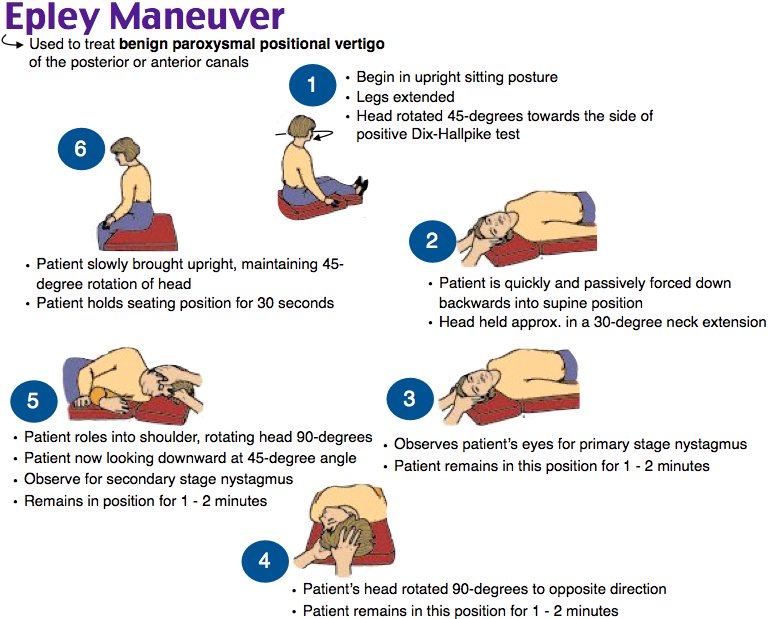
The aim of this study was to perform a randomised, double-blind, sham-controlled clinical trial to evaluate the effectiveness at 1 week, 1 month, and 1 year of a single EM administered by a GP for the treatment of posterior canal BPPV.Īlthough vestibular migraine was not contemplated as an exclusion criterion in the initial trial protocol, growing evidence on the high prevalence of this condition, 17 and its overlapping symptoms with BPPV, alerted the authors to the possibility that patients with vestibular migraine might have been inadvertently enrolled. There have been calls for further research on BPPV in primary care to guide improvements in overall management. Munoz et al 14 reported an improvement in nystagmus (evaluated by the DHT), but not in vertigo symptoms, 1 week after treatment in primary care. There have also been reports of suboptimal management of vertigo and BPPV in this setting due to poor awareness 9 and inadequate use of diagnostic and treatment tools. Little is known about the use of the EM in primary care, even though approximately 60% to 80% of patients with BPPV are first seen by a GP. 7 Numerous systematic reviews have shown that this manoeuvre is an effective treatment for posterior canal BPPV and is superior to observation alone. Posterior canal BPPV is treated using canalith repositioning procedures, the most common of which is the Epley manoeuvre (EM). 5 Such cases are referred to as subjective BPPV, and they have been estimated to account for between 11.5% and 48% of all cases.
Some authors, however, claim that the triggering of vertigo symptoms without demonstration of nystagmus is sufficient for a diagnosis. The diagnosis in such cases is objective BPPV. The diagnostic test for BPPV is the Dix–Hallpike test (DHT), 4 which is considered positive when it triggers vertigo symptoms and torsional delayed nystagmus.
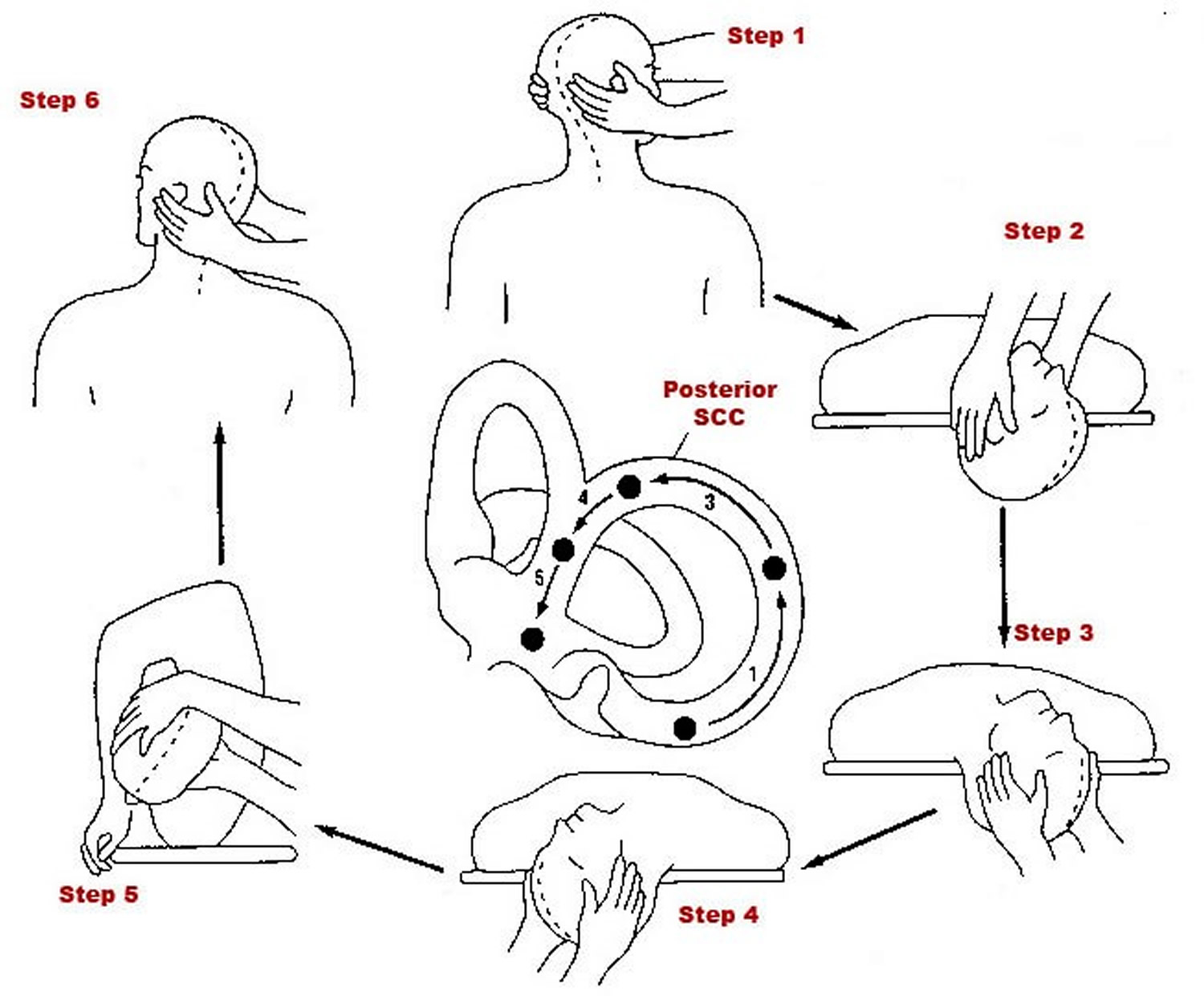
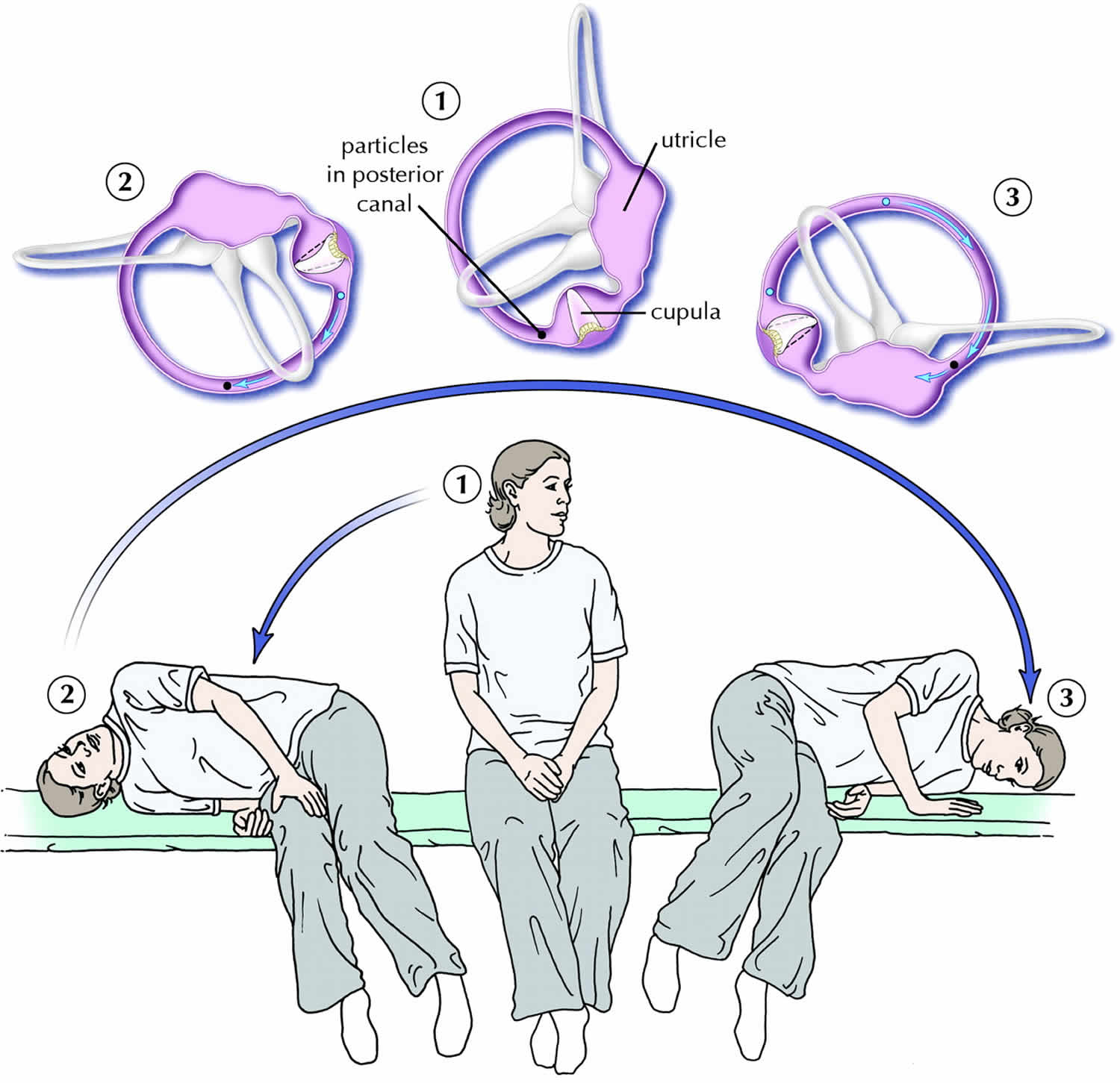
BPPV is caused by the migration of otoconia from the utricular macula to the semicircular canals. It is a subjective sensation precipitated by changes in head position. Patients typically describe BPPV as a transient sensation of spinning surroundings. 2 Approximately 60% to 90% of cases arise in the posterior canal. 1 Benign paroxysmal positional vertigo (BPPV) is the most common type of vertigo and has an estimated lifetime prevalence of 2.4%. Vertigo is a common reason for primary care consultation.
